
How to be Inclusive in Gynecology?
“You can’t be modern if you are not inclusive.” In this article we talk about being inclusive in gynecology.
It was the feedback Aspivix received in social media after releasing its newly created vision statement “Gynecology. Now modern” which was followed by a descriptor: “Developing modern devices in gynecology for clinicians and women.”
Using gender-balanced language is becoming non-optional in every sector, yet how do we articulate inclusiveness in a sector named ‘women’s healthcare’ ?
Such reflections made us stop and recognize the pivotal role of companies in the field of Obstetrics and Gynecology, so we asked ourselves:
- How to be inclusive in gynecology?
- How to approach the special needs of transgender people from a medical perspective?
If you are in the women’s health space, you are likely wondering the same. Take a read a share with us your thought.
Inclusivity and Diversity: Definition and Terminology
Inclusivity is defined by Oxford Languages as “the practice or policy of providing equal access to opportunities and resources for people who might otherwise be excluded or marginalized, such as those having physical or mental disabilities or belonging to other minority groups.”
Similarly, diversity refers to including and involving people from a range of different social and ethnic backgrounds and of different genders and sexual orientations, etc. (1)
In obstetrics and gynecology, where women are known as the primary patients, where do transgender and non-binary patients fit?
In the US, about 1 in every 250 adults is transgender. Transgender is a term used to describe people whose gender identity or expression does not match the sex they were assigned at birth.
Transexuals, people who cross-dress, drag kings and queens, genderqueer or non-binary, non-conforming, and multi-gendered also fall under this umbrella term. (2)
Below are the definitions of some of these categories (3):
- Male to female transgender: Someone whose gender experience is female, but was born with a male body.
- Female to male transgender: Someone whose gender experience is male, but was born with a female body.
- Genderqueer/non-binary: Someone who does not subscribe to conventional gender distinctions but identifies with neither, both, or a combination of male and female genders.
Inclusion in Gynecology from a Medical Perspective
The American College of Obstetricians and Gynecologists (ACOG) has made a statement opposing discrimination based on gender identity and “advocates for inclusive, thoughtful, and affirming care’ for transgenders. (4)
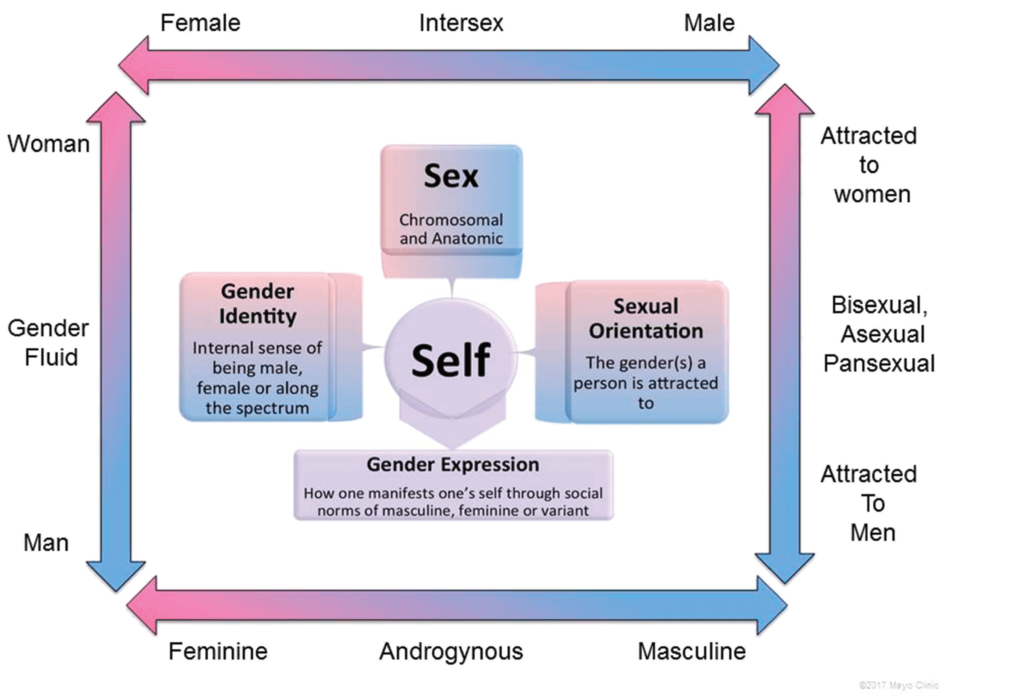
Concepts of sex and gender by Mayo Clinic. Source: acog.org
It is a common mistake to assume that transgenders have undergone gender reassignment surgery, as a patient who considers himself or herself a transgender may still have all of the sexual organs they were born with. (4)
A transgender’s experience when it comes to healthcare may be complicated. Transmen, for example, may still have menstruation. This means they can still be reminded of the female aspects of their body. (3)
Transgenders and gender diverse individuals may consult gynecologists for these concerns:
- fertility,
- pregnancy,
- contraception,
- abortion,
- masculinizing or feminizing hormone therapy/surgery,
- cancer screening, and preventive care. (3)
Regardless of gender or sexuality, it is important to have cervical cancer screenings, contraception, and testing for sexually transmitted infections. (5)
Healthcare for Transgender & Gender Diverse Individuals in OBGYN
To create an inclusive environment for transgenders, here are some recommendations from ACOG:
1. Increase knowledge and comfort with providing care for transgenders and nonconforming individuals. Assumptions should never be made about a patient’s sexual orientation, practices, and surgeries. Healthcare professionals should also only ask questions that are relevant to conditions being treated or to the care being provided.
2. Train all staff on how to appropriately address transgender and gender diverse individuals. The best thing to do here is to ask the patient their name and which pronoun they would like to use. Likewise, clinic staff should also be trained to apologize for mistakes if they occur.
You can ask the patient what name they would like to use and the name on their insurance records, if this is applicable.
3. Take a look at the visuals and educational office used at the clinic or healthcare facility. These images should represent all genders. Also, post a nondiscrimination policy at the clinic.
4. Provide one gender-neutral restroom.
5. In the patient forms, include options for all genders and sexual orientations. Patients may want to also add information that is not asked in the form, so it is a good practice to include blank spaces for other relevant information that the patient may want to add.
While you can ask about the patient’s current gender identity, they should be given the option to choose not to disclose. It is acceptable, however, to ask the sex the patient was assigned at birth.
The national LGBTQIA + Health Education Center has a guide to help healthcare professionals in collecting patient data on sexual orientation and gender identity.
6. Use gender-neutral language. For example, if you want to say “breast / chest,” you can say “upper body.”
Here is some gender-neutral alternatives that refer to male and female anatomy (6) :
- “Genitals” as an alternative for “penis.”
- “Erectile tissue” as an alternative for “clitoris.”
- “Opening of the genitals” instead of “opening of the vagina.”
- “External gonads” to refer to “testes” or “testicles.”
- “Internal gonads” to refer to “ovaries.”
- “Internal reproductive organs” to “female reproductive organs.”
Transcare BC has more examples of gender inclusive language here.
Discussion
As a developer of a novel and “modern” cervical device, at Aspivix we have and feel the responsibility to bring to the table the discussion around Inclusion in Gynecology.
It is critical to actively listen to the voice of our customers and reflect about what are the current needs of everyone involved.
Are you a company in women’s health? How do you approach inclusion in your messaging? Share with us your experience – we would like to hear from you!
Sources:
1. Oxford Languages and Google – English | Oxford Languages (oup.com)
2. Answers to your questions about transgender people, gender identity, and gender expression (apa.org)
3. Transgender healthcare: Guidelines for gynecology providers | MobileODT
4. Health Care for Transgender and Gender Diverse Individuals | ACOG
5. Gynecologic Care for Transgender Patients | CU OB-GYN | Denver, CO (coloradowomenshealth.com)
Share this story:










